Comparative Analysis of Renal Function and Lipid Profile in Diabetic Patients Across Gender, Age, and Glycemic Control: A Cross-sectional Study in Basrah, Iraq
DOI:
https://doi.org/10.54133/ajms.v10i2.2827Keywords:
Diabetes Mellitus, Diabetic Nephropathies, Dyslipidemias, Glycated Hemoglobin AAbstract
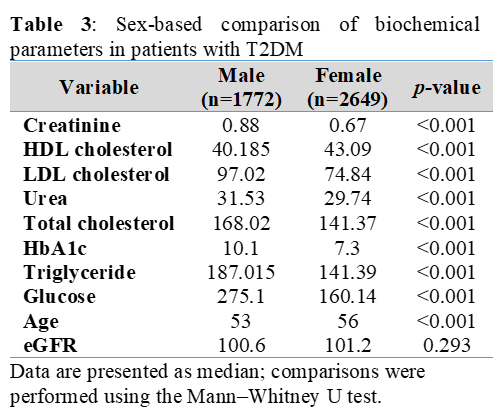
Background: Poor glycemic control adversely affects lipid and renal function; however, the modifying roles of age and sex have not been sufficiently characterized, particularly among Middle Eastern countries. Objective: To evaluate the associations between glycemic control and renal and lipid biomarkers in adults with type 2 diabetes (T2DM) and characterize the independent and combined modulating effects of age and sex. Methods: A cross-sectional comparative study was conducted during 12 months on 4767 subjects attending an outpatient clinic in Basrah, Iraq (4421 with diabetes and 346 with prediabetes). They were grouped according to glycemic control (good: HbA1c<7.0%, suboptimal: 7.0-8.9%, poor: ≥9.0%), age (<40, 40-59, ≥60 years), and gender. Renal function and lipid indexes were analyzed using rank-based tests and regression analysis. Results: Median levels of urea, creatinine, low-density lipoprotein, and triglycerides were significantly higher in the poorly controlled group, whereas HDL levels were lower (p<0.001). Aging is directly related to kidney injury, mainly reduction in eGFR, while male sex is associated with a more atherogenic lipid profile and higher values of renal biomarkers. Multivariate analysis revealed that the impact of age and sex might be disproportionate to, if not greater than, that of HbA1c. Conclusions: In T2DM, the relationship between renal and lipid abnormalities is sex asymmetrical, age-dependent, and glycemic-control-influenced. A personalized, demography-integrated strategy for complication assessment should be adopted to improve diabetic care.
Downloads
References
Yameny AA. Diabetes mellitus overview 2024. J Biosci Appl Res. 2024;10(3):641-645. doi: 10.21608/jbaar.2024.382794. DOI: https://doi.org/10.21608/jbaar.2024.382794
Sun H, Saeedi P, Karuranga S, Pinkepank M, Ogurtsova K, Duncan BB, et al. IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res Clin Pract. 2022;183:109119. doi: 10.1016/j.diabres.2021.109119. DOI: https://doi.org/10.1016/j.diabres.2021.109119
Huang X, Wu Y, Ni Y, Xu H, He Y. Global, regional, and national burden of type 2 diabetes mellitus caused by high BMI from 1990 to 2021, and forecasts to 2045: analysis from the global burden of disease study 2021. Front Public Health. 2025;13:1515797. doi: 10.3389/fpubh.2025.1515797. DOI: https://doi.org/10.3389/fpubh.2025.1515797
Almalki WH, Khan MS. Burden of diabetes mellitus on health and economy of the Arab world: current situation and perspectives. J Public Health (Berl). 2025;1-20. doi: 10.1007/s10389-025-02448-7. DOI: https://doi.org/10.1007/s10389-025-02448-7
Mezil SA, Abed BA. Complications of diabetes mellitus. Ann Romanian Soc Cell Biol. 2021;25(3):1546-1556.
Di Marco M, Scilletta S, Miano N, Marrano N, Natalicchio A, Giorgino F, et al. Cardiovascular risk and renal injury profile in subjects with type 2 diabetes and non-albuminuric diabetic kidney disease. Cardiovasc Diabetol. 2023;22(1):344. doi: 10.1186/s12933-023-02065-2. DOI: https://doi.org/10.1186/s12933-023-02065-2
Ballena-Caicedo J, Zuzunaga-Montoya FE, Loayza-Castro JA, Vásquez-Romero LE, Tapia-Limonchi R, De Carrillo CI, et al. Global prevalence of dyslipidemias in the general adult population: a systematic review and meta-analysis. J Health Popul Nutr. 2025;44(1):308. doi: 10.1186/s41043-025-01054-3. DOI: https://doi.org/10.1186/s41043-025-01054-3
Hashempour Z, Esmaeili F, Tabatabaei-Malazy O, Mosallanejad A, Panahi G. Worldwide prevalence of dyslipidemia in diabetes: an umbrella overview of meta-analyses. Endocr Metab Immune Disord Drug Targets. 2024;24(5):1-12. doi: 10.2174/0118715303375795250521041740. DOI: https://doi.org/10.2174/0118715303375795250521041740
Vesković M, Šutulović N, Hrnčić D, Stanojlović O, Macut D, Mladenović D. The interconnection between hepatic insulin resistance and metabolic dysfunction-associated steatotic liver disease: the transition from an adipocentric to liver-centric approach. Curr Issues Mol Biol. 2023;45(11):9084-9102. doi: 10.3390/cimb45110570. DOI: https://doi.org/10.3390/cimb45110570
Pal SC, Méndez-Sánchez N. Insulin resistance and adipose tissue interactions as the cornerstone of metabolic (dysfunction)-associated fatty liver disease pathogenesis. World J Gastroenterol. 2023;29(25):3999. doi: 10.3748/wjg.v29.i25.3999. DOI: https://doi.org/10.3748/wjg.v29.i25.3999
Khan AW, Jandeleit-Dahm KA. Atherosclerosis in diabetes mellitus: novel mechanisms and mechanism-based therapeutic approaches. Nat Rev Cardiol. 2025. doi: 10.1038/s41569-024-01115-w. DOI: https://doi.org/10.1038/s41569-024-01115-w
Ramadhan HH, Mohammed RN. Biomarkers and the identification of kidney damage in patients with diabetes mellitus. Hilla Univ Coll J Med Sci. 2024;2(4):41-51. doi: 10.62445/2958-4515.1037. DOI: https://doi.org/10.62445/2958-4515.1037
Ullah W, Nazir A, Israr H, Hussain S, Farooq M. Assessment of serum urea and creatinine levels in diabetic patients. BioSci Rev. 2023;5(3):26-32. doi: 10.32350/BSR.53.03. DOI: https://doi.org/10.32350/BSR.53.03
Alidrisi HA, Al-Ibadi AA, Al-Saidi JS, Alsawad MA, Jameel AA, Al-Shati AW, et al. Comparative analysis of glycemic and lipid profiles in newly diagnosed males and females with type 2 diabetes mellitus. Cureus. 2023;15(12). doi: 10.7759/cureus.50101. DOI: https://doi.org/10.7759/cureus.50101
Nnakenyi ID, Nnakenyi EF, Parker EJ, Uchendu NO, Anaduaka EG, Ezeanyika LU. Relationship between glycaemic control and lipid profile in type 2 diabetes mellitus patients in a low-resource setting. Pan Afr Med J. 2022; 41:281. doi: 10.11604/pamj.2022.41.281.33802. DOI: https://doi.org/10.11604/pamj.2022.41.281.33802
Alzahrani SH, Baig M, Aashi MM, Al-Shaibi FK, Alqarni DA, Bakhamees WH. Association between glycated hemoglobin (HbA1c) and the lipid profile in patients with type 2 diabetes mellitus at a tertiary care hospital: a retrospective study. Diabetes Metab Syndr Obes. 2019;12:1639-1644. doi: 10.2147/DMSO.S222271. DOI: https://doi.org/10.2147/DMSO.S222271
Du T, Yuan G, Zhou X, Sun X. Sex differences in the effect of HbA1c-defined diabetes on a wide range of cardiovascular disease risk factors. Ann Med. 2016;48(1-2):34-41. doi: 10.3109/07853890.2015.1127406. DOI: https://doi.org/10.3109/07853890.2015.1127406
Alnidawi BF. Association between glycemic control and serum lipid profile in type 2 diabetic patients: glycated hemoglobin as a dual biomarker. Al-Kindy Coll Med J. 2015;11(2):10-14.
Mansour AA, Alibrahim NT, Alidrisi HA, Alhamza AH, Almomin AM, Zaboon IA, et al. Prevalence and correlation of glycemic control achievement in patients with type 2 diabetes in Iraq: a retrospective analysis of a tertiary care database over 9 years. Diabetes Metab Syndr. 2020;14(3):265-272. doi: 10.1016/j.dsx.2020.03.008. DOI: https://doi.org/10.1016/j.dsx.2020.03.008
Alidrisi HA, Reman KA, Alhubaish ES, Hussein IH, Nwayyir HA, Zaboon IA, et al. Prevalence of chronic kidney disease and associated risk factors in patients with type 2 diabetes mellitus in Basrah, Iraq: a cross-sectional study. Diabetes Epidemiol Manag. 2026;100301. doi: 10.34172/aim.31194. DOI: https://doi.org/10.1016/j.deman.2026.100301
Vergès B. Pathophysiology of diabetic dyslipidemia: where are we? Diabetologia. 2015;58(5):886-899. doi: 10.1007/s00125-015-3525-8. DOI: https://doi.org/10.1007/s00125-015-3525-8
American Diabetes Association Professional Practice Committee. Cardiovascular disease and risk management: Standards of medical care in diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S190-S212. doi: 10.2337/dc24-S010. DOI: https://doi.org/10.2337/dc24-S010
Stefanovski D, Punjabi NM, Boston RC, Watanabe RM. Insulin action, glucose homeostasis, and free fatty acid metabolism: insights from a novel model. Front Endocrinol (Lausanne). 2021;12:625701. doi: 10.3389/fendo.2021.625701. DOI: https://doi.org/10.3389/fendo.2021.625701
Frühbeck G, Méndez-Giménez L, Fernández-Formoso JA, Fernández S, Rodríguez A. Regulation of adipocyte lipolysis. Nutr Res Rev. 2014;27(1):63-93. doi: 10.1017/S095442241400002X. DOI: https://doi.org/10.1017/S095442241400002X
Mir MM, Jeelani M, Alharthi MH, Rizvi SF, Sohail SK, Wani JI, et al. Unraveling the mystery of insulin resistance: from principal mechanistic insights and consequences to therapeutic interventions. Int J Mol Sci. 2025;26(6):2770. doi: 10.3390/ijms26062770. DOI: https://doi.org/10.3390/ijms26062770
Chakraborty S, Verma A, Garg R, Singh J, Verma H. Cardiometabolic risk factors associated with type 2 diabetes mellitus: a mechanistic insight. Clin Med Insights Endocrinol Diabetes. 2023;16. doi: 10.1177/11795514231220780. DOI: https://doi.org/10.1177/11795514231220780
Ginsberg HN, Packard CJ, Chapman MJ, Borén J, Aguilar-Salinas CA, Averna M, et al. Triglyceride-rich lipoproteins and their remnants: metabolic insights, role in atherosclerotic cardiovascular disease, and emerging therapeutic strategies. Eur Heart J. 2021;42(47):4791-4806. doi: 10.1093/eurheartj/ehab551. DOI: https://doi.org/10.1093/eurheartj/ehab551
Hirano T. Pathophysiology of diabetic dyslipidemia. J Atheroscler Thromb. 2018;25(9):771-782. doi: 10.5551/jat.RV17023. DOI: https://doi.org/10.5551/jat.RV17023
Afkarian M, Sachs MC, Kestenbaum B, Hirsch IB, Tuttle KR, Himmelfarb J, et al. Kidney disease and increased mortality risk in type 2 diabetes. J Am Soc Nephrol. 2013;24(2):302-308. doi: 10.1681/ASN.2012070718. DOI: https://doi.org/10.1681/ASN.2012070718
Van Raalte DH, Bjornstad P, Cherney DZ, de Boer IH, Fioretto P, Gordin D, et al. Combination therapy for kidney disease in people with diabetes mellitus. Nat Rev Nephrol. 2024;20(7):433-446. doi: 10.1038/s41581-024-00827-z. DOI: https://doi.org/10.1038/s41581-024-00827-z
Delanaye P, Cavalier E, Stehlé T, Pottel H. Glomerular filtration rate estimation in adults: myths and promises. Nephron. 2024;148(6):408-414. doi: 10.1159/000536243. DOI: https://doi.org/10.1159/000536243
Khader NA, Kamath VG, Kamath SU, Rao IR, Prabhu AR. Kidney function estimation equations: a narrative review. Ir J Med Sci. 2025;194(2):725-743. doi: 10.1007/s11845-025-03874-y. DOI: https://doi.org/10.1007/s11845-025-03874-y
Wang Y, O Neil A, Jiao Y, Wang L, Huang J, Lan Y, et al. Sex differences in the association between diabetes and risk of cardiovascular disease, cancer, and mortality: a systematic review and meta-analysis. BMC Med. 2019;17(1):136. doi: 10.1186/s12916-019-1355-0. DOI: https://doi.org/10.1186/s12916-019-1355-0
Amani-Beni R, Darouei B, Zefreh H, Sheikhbahaei E, Sadeghi M. Effect of obesity duration and BMI trajectories on cardiovascular disease: a narrative review. Cardiol Ther. 2023;12(2):307-326. doi: 10.1007/s40119-023-00317-6. DOI: https://doi.org/10.1007/s40119-023-00317-6
Siddiqui A, Gill R, Ringor M, Dugal JK, Malhi A, Abdallah A, et al. Gender disparities in coronary artery disease: a review of factors influencing clinical outcomes. Neth Heart J. 2025. doi: 10.1007/s12471-025-01996-7. DOI: https://doi.org/10.1007/s12471-025-01996-7
Dybiec J, Szlagor M, Młynarska E, Rysz J, Franczyk B. Structural and functional changes in aging kidneys. Int J Mol Sci. 2022;23(23):15435. doi: 10.3390/ijms232315435. DOI: https://doi.org/10.3390/ijms232315435
Noronha IL, Santa-Catharina GP, Andrade L, Coelho VA, Jacob-Filho W, Elias RM. Glomerular filtration in the aging population. Front Med (Lausanne). 2022;9:769329. doi: 10.3389/fmed.2022.769329. DOI: https://doi.org/10.3389/fmed.2022.769329
Wang Q, Pang D, Wang H. Effect of overall lifestyle on mortality and cardiovascular disease death in dyslipidemia patients. BMC Cardiovasc Disord. 2023;23(1):438. doi: 10.1186/s12872-023-03450-1. DOI: https://doi.org/10.1186/s12872-023-03450-1
Andersson NW, Corn G, Dohlmann TL, Melbye M, Wohlfahrt J, Lund M. LDL-C reduction with lipid-lowering therapy for primary prevention of major vascular events among older individuals. J Am Coll Cardiol. 2023;82(14):1381-1391. doi: 10.1016/j.jacc.2023.07.027. DOI: https://doi.org/10.1016/j.jacc.2023.07.027
Hou Y, Hu Z, Jiang F, Zhao Q, Wang C, Zhang Y. Gender-specific health-adjusted life expectancy of type 2 diabetes mellitus among the rural elderly population. Int J Public Health. 2024;69:1606680. doi: 10.3389/ijph.2024.1606680. DOI: https://doi.org/10.3389/ijph.2024.1606680
Lacasse A, Nguefack HL, Page MG, Choinière M, Samb OM, Katz J, et al. Sex and gender differences in healthcare utilization trajectories: a cohort study among Quebec workers living with chronic pain. BMJ Open. 2023;13(7):e070509. doi: 10.1136/bmjopen-2022-070509. DOI: https://doi.org/10.1136/bmjopen-2022-070509
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Al-Rafidain Journal of Medical Sciences ( ISSN 2789-3219 )

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Published by Al-Rafidain University College. This is an open access journal issued under the CC BY-NC-SA 4.0 license (https://creativecommons.org/licenses/by-nc-sa/4.0/).











