Physician Adherence to Treatment Guidelines and the Incidence of Prescribing Errors for Patients in Intensive and Cardiac Care Units at a Teaching Hospital, Al-Muthanna City, Iraq: A Retrospective Analysis
DOI:
https://doi.org/10.54133/ajms.v10i1.2677Keywords:
Cardiac care unit, Critical care unit, Intensive care unit, Iraqi hospitals, Prescribing errorsAbstract
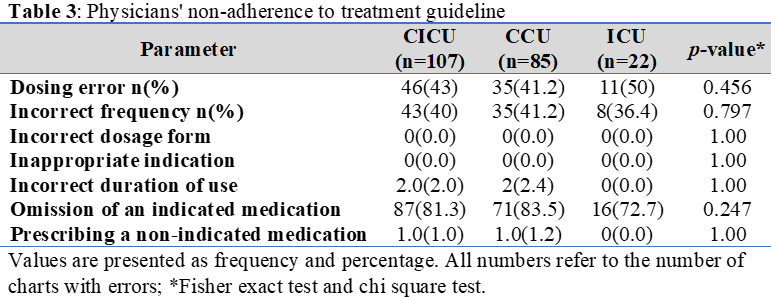
Background: Prescribing errors are common worldwide. They are exposing critically ill patients to increased morbidity and mortality and overwhelming healthcare systems. Limited data exist on the prevalence of prescribing errors for critically ill patients in Iraq. Objectives: To assess the prevalence and types of prescribing errors in the Cardiac and Intensive Care Units in Iraq. Methods: A retrospective study was conducted at a teaching hospital in Al-Muthanna, Iraq. Charts of patients admitted to the Cardiac and Intensive Care Units for at least one day between January and June 2024 were included, excluding those without a diagnosis. To detect prescribing errors, the latest American guidelines, the British National Formulary, and Medscape were used. Results: Out of 239 charts included, 107 showed prescribing errors. Patients were prescribed 7.66±2.32 medications. Meanwhile, 2.29±1.17 of them contain an error. Omission of indicated medications (81.3%) and dosing errors (43%) were detected due to non-adherence to treatment guidelines. Lack of monitoring for prescribed medications (59.8%) and prescribing drug-drug interactions (31.8%) were also common. The number of diseases and renal impairments was positively correlated with the frequency of errors. Patient age, medical history, renal function, number of medications, and errors didn't significantly impact patients' mortality. Conclusions: Prescribing errors are prevalent in the cardiac ICU, mainly due to poor adherence to treatment guidelines. Despite the presence of errors, no significant relationship was reported between prescribing errors and patients' mortality.
Downloads
References
Amalia AE, Basabih M. Overview of medication error incidence in hospitals in various countries: Literature review. Indones J Health Admin. 2023;11(1):145-53.doi: 10.20473/jaki.v11i1.2023.145-153. DOI: https://doi.org/10.20473/jaki.v11i1.2023.145-153
Mosah HA, Sahib AS, AL-Biati HA. Evaluation of medication errors in hospitalized patients. Al-Kindy Col Med J. 2012;8(2):75-79.
Mistry B, Patel Z, Prajapati M. Medication errors: understanding the types, causes, and prevention, and the critical role of pharmacists. Int J Pharm Res App. 2023;8(5):1358-1370. doi.10.35629/7781-080513581370.
Tsegaye D, Alem G, Tessema Z, Alebachew W. Medication administration errors and associated factors among nurses. Int J Gen Med. 2020:1621-32.Doi:10.2147/IJGM.S289452. DOI: https://doi.org/10.2147/IJGM.S289452
Gala P, Rathod D, Patel M. Critical illness & medication errors. Int J Health Res. 2025;15(1):219-223. doi: 10.52403/ijhsr.20250128. DOI: https://doi.org/10.52403/ijhsr.20250128
Nassehi A, Jafari M, Rashvand F, Rafiei H, Hosseinpour F, Shamekhi L. Intensive care unit, cardiac care unit, and emergency department nurses' perceptions of medical device-related pressure injuries: a cross-sectional study. Wound Manag Prev. 2022;68(9):24-28. doi:10.25270/wmp.2022.9.2428. DOI: https://doi.org/10.25270/wmp.2022.9.2428
Kwiecień-Jaguś K, Mędrzycka-Dąbrowska W, Kopeć M. Understanding medication errors in intensive care settings and operating rooms—A Systematic review. Medicina. 2025;61(3):369.doi: 10.3390/medicina61030369. DOI: https://doi.org/10.3390/medicina61030369
Freedman JE, Becker RC, Adams JE, Borzak S, Jesse RL, Newby LK, et al. Medication errors in acute cardiac care: An American Heart Association scientific statement from the council on clinical cardiology subcommittee on acute cardiac care, council on cardiopulmonary and critical care, council on cardiovascular nursing, and council on stroke. Circulation. 2002;106(20):2623-2629. doi: 10.1161/01.cir.0000037748.19282.7d. DOI: https://doi.org/10.1161/01.CIR.0000037748.19282.7D
Pintado Delgado MC, Sánchez Navarro IM, BaldominosUtrilla G. Medication errors reported in an adult Intensive Care Unit in a level 2 hospital in Spain. Med Intensiva (Engl Ed). 2023;47(12):736-738. doi: 10.1016/j.medine.2023.10.003. DOI: https://doi.org/10.1016/j.medine.2023.10.003
Alsulami Z, Conroy S, Choonara I. Medication errors in the Middle East countries: A systematic review of the literature. Eur J ClinPharmacol. 2013;69(4):995-1008. Doi: 10.1007/s00228-012-1435-y. DOI: https://doi.org/10.1007/s00228-012-1435-y
Bakhshi F, Mitchell R, Khosravi A, Antikchi M. Guideline adherence for controlling incidence of medication errors: a systematic mixed-method review. Int J Pharm Pract. 2025:riaf049. doi: 10.1093/ijpp/riaf049. DOI: https://doi.org/10.1093/ijpp/riaf049
EscrivaGracia J, AparisiSanz A, Brage Serrano R, Fernandez Garrido J. Medication errors and risk areas in a critical care unit. J AdvNurs. 2021;77(1):286-295. doi:10.1111/JAN.14612. DOI: https://doi.org/10.1111/jan.14612
Kumar M, Sahni N, Shafiq N, Yaddanapudi LN. Medication prescription errors in the intensive care unit: prospective observational study. Indian J Crit Care Med. 2022;26(5):555-559. doi: 10.5005/jp-journals-10071-24148. DOI: https://doi.org/10.5005/jp-journals-10071-24148
Aidah S, Gillani SW, Alderazi A, Abdulazeez F. Medication error trends in Middle Eastern countries: A systematic review on healthcare services. J Educ Health Promot. 2021;10(1):227.doi:10.4103/jehp.jehp_1549_20. DOI: https://doi.org/10.4103/jehp.jehp_1549_20
Anwer IY, Yawuz MJ, Al-Jumaili AA. In-depth assessment of Iraqi physicians' adherence to treatment guidelines for different diseases: a qualitative study. F1000Research. 2024;12(350):350.doi:10.12688/f1000research.128233.1. DOI: https://doi.org/10.12688/f1000research.128233.2
Joint Formulary Committee. British National Formulary,( 84th ed.), London:BMJ Group and Pharmaceutical Press;2022.
Safavi KC, Dharmarajan K, Kim N, Strait KM, Li SX, Chen SI, et al. Variation exists in rates of admission to intensive care units for heart failure patients across hospitals in the United States. Circulation. 2013;127(8):923-929.doi: 10.1161/Circulationaha.112.001088. DOI: https://doi.org/10.1161/CIRCULATIONAHA.112.001088
Bohula EA, Katz JN, van Diepen S, Alviar CL, Baird-Zars VM, Park JG, et al. Demographics, care patterns, and outcomes of patients admitted to cardiac intensive care units: the Critical Care Cardiology Trials Network Prospective North American Multicenter Registry of Cardiac Critical Illness. JAMA Cardiol. 2019;4(9):928-935. doi: 10.1001/jamacardio.2019.2467. DOI: https://doi.org/10.1001/jamacardio.2019.2467
Sikandar MZ, Khan MAW, Khan AA, Javed M, Moeen SMH, Asghar A. Assessment of causes of intensive care unit admissions in renal disease patients: A cross-sectional study. BiolClinSci Res J. 2023;2023(1):612. doi: 10.54112/bcsrj.v2023i1.612. DOI: https://doi.org/10.54112/bcsrj.v2023i1.612
Fidalgo P, Bagshaw SM. Chronic kidney disease in the intensive care unit. Manag Chronic Kidney Dis. 2014:417:38. doi: 10.1007/978-3-642-54637-2_32. DOI: https://doi.org/10.1007/978-3-642-54637-2_32
Mittal N, Verma M, Siwach S, Bansal P, Singhal SK. Drug utilization research and predictors of outcomes in the intensive care unit of a tertiary care hospital: A prospective observational study. Cureus. 2023;15(12). doi: 10.7759/cureus.50653. DOI: https://doi.org/10.7759/cureus.50653
Nagabushan H, Roopadevi HS, Prakash GM, Pankaja R. A prospective study of drug utilization pattern in cardiac intensive care unit at a tertiary care teaching hospital. Int J Basic ClinPharmacol. 2017;4(3);579–583. doi: 10.18203/2319-2003.ijbcp20150044. DOI: https://doi.org/10.18203/2319-2003.ijbcp20150044
Alanazi WK, Almutairi SH, Alamri AA, Alsubaie MF, Tohary OM, Hussein MT, et al. Effect of electronic prescription system modifications on reducing prescribing errors in a military hospital. J Pharm Policy Pract. 2024;17(1):2431177. doi: 10.1080/20523211.2024.2431177. DOI: https://doi.org/10.1080/20523211.2024.2431177
Merino P, Martín MC, Alonso A, Gutiérrez I, Alvarez J, Becerril F. Medication errors in Spanish intensive care units. Med Intensiva. 2013;37(6):391-399. doi: 10.1016/j.medin.2012.11.002. DOI: https://doi.org/10.1016/j.medine.2012.11.004
Laher AE, Enyuma CO, Gerber L, Buchanan S, Adam A, Richards GA, et al. Medication errors at a tertiary hospital intensive care unit. Cureus. 2021;13(12). doi: 10.7759/cureus.20374. DOI: https://doi.org/10.7759/cureus.20374
Al Hilfi TK, Lafta R, Burnham G. Health services in Iraq. Lancet. 2013;381(9870):939-948. doi: 10.1016/S0140-6736(13)60320-7. DOI: https://doi.org/10.1016/S0140-6736(13)60320-7
Nassrullah Z, Al-Jumaili AA. Professional challenges facing pharmacists working at public hospitals in an Iraqi province: A qualitative study. Iraqi J Pharm Sci. 2023;32(Suppl.):204-213. doi: 10.31351/vol32issSuppl.pp204-213. DOI: https://doi.org/10.31351/vol32issSuppl.pp204-213
Ajemigbitse AA, Omole MK, Erhun WO. Effect of providing feedback and prescribing education on prescription writing: An intervention study. Ann Afr Med. 2016;15(1):1-6. doi: 10.4103/1596-3519.161722. DOI: https://doi.org/10.4103/1596-3519.161722
Shahmoradi L, Safdari R, Ahmadi H, Zahmatkeshan M. Clinical decision support systems-based interventions to improve medication outcomes: A systematic literature review on features and effects. Med J Islam Repub Iran. 2021;35:27. doi: 10.47176/mjiri.35.27. DOI: https://doi.org/10.47176/mjiri.35.27
El-Bosily HM, Abd El Meguid KR, Sabri NA, Ahmed MA. Physicians' adherence to evidence-based guidelines as a major predictor of anticoagulant-related medication error incidence and severity. Br J ClinPharmacol. 2022;88(8):3730-3740. doi: 10.1111/bcp.15314. DOI: https://doi.org/10.1111/bcp.15314
Salih N, Kadhim D. Adherence to American Society of Health-System Pharmacists surgical antibiotic prophylaxis guideline in medical city teaching hospitals/Baghdad. Iraqi J Pharm Sci. 2016;25:2016. doi:10.31351/ vol25iss2pp40-45.
Sada O, Melkie A, Shibeshi W. Medication prescribing errors in the medical intensive care unit of TikurAnbessa Specialized Hospital, Addis Ababa, Ethiopia. BMC Res Notes. 2015;8(1):448. doi: 10.1186/s13104-015-1435-y. DOI: https://doi.org/10.1186/s13104-015-1435-y
Agalu A, Ayele Y, Bedada W, Woldie M. Medication prescribing errors in the intensive care unit of Jimma University Specialized Hospital, Southwest Ethiopia. J MultidiscipHealthc. 2011:377-382. doi: 10.2147/JMDH.S24671. DOI: https://doi.org/10.2147/JMDH.S24671
Alyami MH, Naser AY, Alswar HS, Alyami HS, Alyami AH, Al Sulayyim HJ. Medication errors in Najran, Saudi Arabia: Reporting, responsibility, and characteristics: A cross-sectional study. Saudi Pharm J. 2022;30(4):329-336. doi: 10.1016/j.jsps.2022.02.005. DOI: https://doi.org/10.1016/j.jsps.2022.02.005
Avery T, Gookey G, Spencer R, Knox R, Marsden K, Salema N. Providing the right medication monitoring. InnovAiT. 2013;6(8):515-523. doi: 10.1177/1755738013494368. DOI: https://doi.org/10.1177/1755738013494368
Ewoldt TMJ, Abdulla A, van, Hunfeld N, Soma Bahmany, Muller AE, et al.. Barriers and facilitators for therapeutic drug monitoring of beta-lactams and ciprofloxacin in the ICU: a nationwide cross-sectional study. BMC Infect Dis. 2022;22(1):611.Doi: 10.1186/s12879-022-07587-w. DOI: https://doi.org/10.1186/s12879-022-07587-w
Pote S, Tiwari P, D'cruz S. Medication prescribing errors in a public teaching hospital in India: A prospective study. Pharm Pract (Granada). 2007;5(1):17-20. doi: 10.4321/s1886-36552007000100003. DOI: https://doi.org/10.4321/S1886-36552007000100003
Al-Jumaili AA, Jabri AM, Al-Rekabi MD, Abbood SK, Hussein AH. Physician acceptance of pharmacist recommendations about medication prescribing errors in Iraqi hospitals. Innov Pharmacy. 2016;7. doi: 10.24926/iip.v7i3.443. DOI: https://doi.org/10.24926/iip.v7i3.443
Chen YF, Neil KE, Avery AJ, Dewey ME, Johnson C. Prescribing errors and other problems reported by community pharmacists. TherClin Risk Manag. 2005;1(4):333-342.
Milani RV, Oleck SA, Lavie CJ. Medication errors in patients with severe chronic kidney disease and acute coronary syndrome: the impact of computer-assisted decision support. Mayo Clin Proc. 2011;86(12):1161–1164. doi: 10.4065/mcp.2011.0290. DOI: https://doi.org/10.4065/mcp.2011.0290
Papotti B, Marchi C, Adorni MP, Potì F. Drug-drug interactions in polypharmacy patients: The impact of renal impairment. Curr Res Pharmacol Drug Discov. 2021;2:100020. doi: 10.1016/j.crphar.2021.100020. DOI: https://doi.org/10.1016/j.crphar.2021.100020
Rasool MF, Rehman AU, Imran I, Abbas S, Shah S, Abbas G, et al. Risk factors associated with medication errors among patients suffering from chronic disorders. Front Public Health. 2020;8:531038. doi: 10.3389/fpubh.2020.531038. DOI: https://doi.org/10.3389/fpubh.2020.531038
Kır S, Bahçeci BK, Ayrancı E, Balkoca M, Çolak ÖY, Ayrancı E, et al. Age is not a risk factor in survival of severely ill patients with co-morbidities in a medical intensive care unit. Ir J Med Sci. 2021;190(1):317-324. doi: 10.1007/s11845-020-02298-0. DOI: https://doi.org/10.1007/s11845-020-02298-0
de Rooij SE, Abu-Hanna A, Levi M, de Jonge E. Factors that predict outcome of intensive care treatment in very elderly patients: a review. Crit Care. 2005;9(4):R307. doi: 10.1186/cc3536. DOI: https://doi.org/10.1186/cc3536
Perreault S, Schnitzer ME, Disso E, Qazi J, Boivin-Proulx LA, Dorais M. Polypharmacy and risk of mortality among patients with heart failure following hospitalization: A nested case–control study. Sci Rep. 2022;12(1):19963.doi: 10.1038/s41598-022-24285-4. DOI: https://doi.org/10.1038/s41598-022-24285-4
Lenti MV, Croce G, Brera AS, Ballesio A, Padovini L, Bertolino G, et al. Rate and risk factors of in-hospital and early post-discharge mortality in patients admitted to an internal medicine ward. Clin Med. 2023;23(1):16–23. doi: 10.7861/clinmed.2022-0176. DOI: https://doi.org/10.7861/clinmed.2022-0176
Melaku EE, Urgie BM, Dessie F, Seid A, Abebe Z, Tefera AS. Determinants of mortality of patients admitted to the intensive care unit at DebreBerhan Comprehensive Specialized Hospital: A retrospective cohort study. Patient Relat Outcome Meas. 2024:61-70. doi: 10.2147/PROM.S450502. DOI: https://doi.org/10.2147/PROM.S450502
Atmaja DS, Saksono RY, Yulistiani, Suharjono, Zairina E. Evaluation of medication errors in one of the largest public hospital: A retrospective study. ClinEpidemiol Glob Health. 2024;28:101640-0. doi: 10.1016/j.cegh.2024.101640. DOI: https://doi.org/10.1016/j.cegh.2024.101640
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Al-Rafidain Journal of Medical Sciences ( ISSN 2789-3219 )

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Published by Al-Rafidain University College. This is an open access journal issued under the CC BY-NC-SA 4.0 license (https://creativecommons.org/licenses/by-nc-sa/4.0/).











