Association of Dialysis Adequacy with Health-Related Quality of Life Among Maintenance Hemodialysis Patients: A Cross-Sectional Study
DOI:
https://doi.org/10.54133/ajms.v10i1.2439Keywords:
Adequacy, Hemodialysis, Health-related quality of life, PatientsAbstract
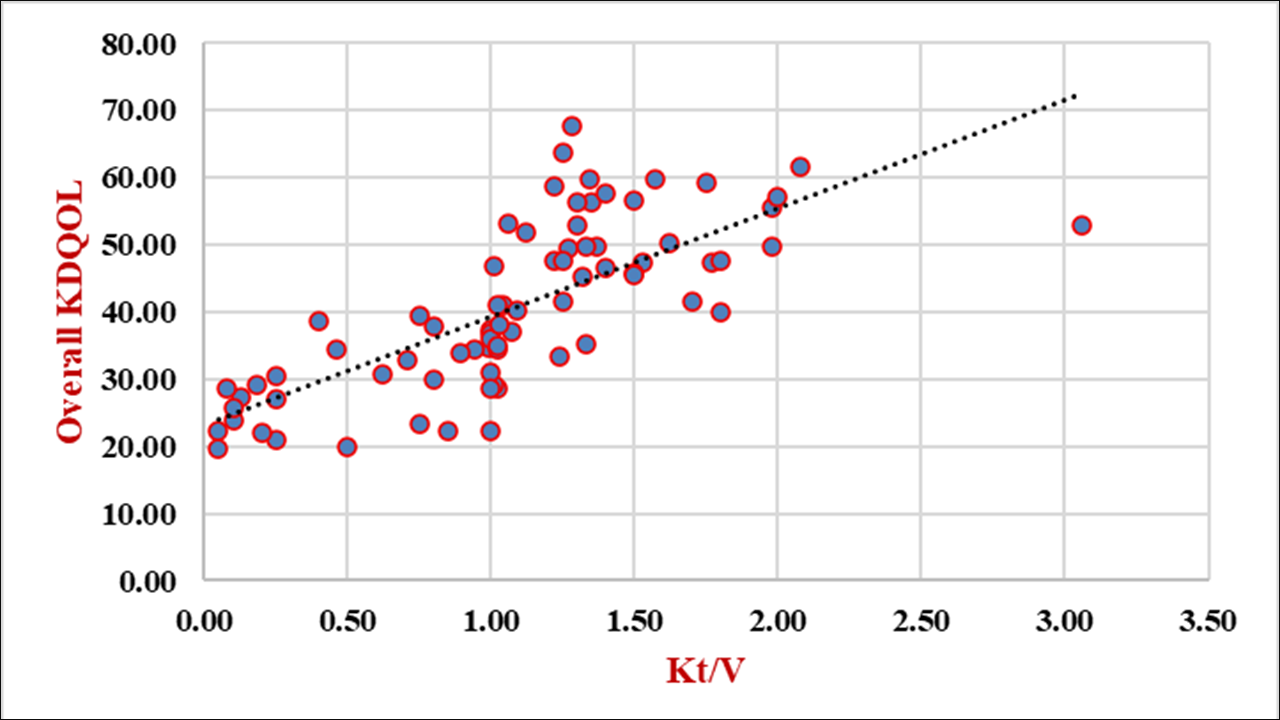
Background: Hemodialysis is used as renal replacement treatment to extend patients' lives. Adequate and effective dialysis can improve patients’ quality of life; however, there is a lack of data regarding dialysis adequacy and its impact on quality of life (QOL) among hemodialysis patients in the Yemeni context. Objective: To assess the association between dialysis adequacy and health‑related quality of life (HRQOL) among hemodialysis patients. Methods: A descriptive cross-sectional study was conducted among 77 patients selected from the hemodialysis center of the 22 May Hospital Authority in Amran City, Yemen, from December 2024 to April 2025, using a convenience sampling method. Data were collected through face-to-face interviews using a validated Arabic version of the Kidney Disease Quality of Life (KDQOL™-36) questionnaire and by measuring dialysis adequacy (Kt/V) according to standardized procedures. Results: This study showed 58.4% of patients received inadequate dialysis, and 41.6% achieved adequate dialysis based on KT/V values. The mean KDQOL score was 40.66, highest for symptoms/problems (49.11) and lowest for burden of kidney disease (25.65). Patients with adequate dialysis had significantly better scores for symptom/problem, effect, and burden subscales. Dialysis adequacy correlated positively with overall HRQOL (r=0.54, p<0.001). Hemoglobin >10 g/dL was also linked to higher HRQOL (p=0.006). Conclusions: Most HD patients experienced inadequate dialysis and impaired HRQOL. Dialysis adequacy and anemia control emerged as key determinants of better HRQO.
Downloads
References
Balouchi A, Parvizy S, Nia HS, Ebadi A. Dialysis adequacy among haemodialysis patients in Eastern Mediterranean region: A systematic review and meta-analysis. Asia Pacific J Health Manag. 2021;16(4). doi: 10.24083/apjhm.v16i4.1139. DOI: https://doi.org/10.24083/apjhm.v16i4.1139
Liyanage T, Toyama T, Hockham C, Ninomiya T, Perkovic V, Woodward M, et al. Prevalence of chronic kidney disease in Asia: A systematic review and analysis. BMJ Glob Health. 2022;7(1). doi: 10.1136/bmjgh-2021-007525. DOI: https://doi.org/10.1136/bmjgh-2021-007525
Ke C, Liang J, Liu M, Liu S, Wang C. Burden of chronic kidney disease and its risk-attributable burden in 137 low-and middle-income countries, 1990–2019: results from the global burden of disease study 2019. BMC Nephrol. 2022;23(1). doi: 10.1186/s12882-021-02597-3. DOI: https://doi.org/10.1186/s12882-021-02597-3
Ravindran A, Sunny A, Kunnath RP, Divakaran B. Assessment of quality of life among end-stage renal disease patients undergoing maintenance hemodialysis. Indian J Palliat Care. 2020;26(1):47–53. doi: 10.4103/IJPC.IJPC_141_19. DOI: https://doi.org/10.4103/IJPC.IJPC_141_19
Himmelfarb J, Vanholder R, Mehrotra R, Tonelli M. The current and future landscape of dialysis. Nat Rev Nephrol. 2020;16(10):573-585. doi: 10.1038/s41581-020-0315-4. DOI: https://doi.org/10.1038/s41581-020-0315-4
Yasin F, Khraim F, Santos M, Forgrave D, Hamad A. Factors influencing self-care management in adult hemodialysis patients: An integrative review. Qatar Med J. 2024;2024(1). doi: 10.5339/qmj.2024.12. DOI: https://doi.org/10.5339/qmj.2024.12
Al Salmi I, Kamble P, Lazarus ER, D’Souza MS, Al Maimani Y, Hannawi S. Kidney disease-specific quality of life among patients on hemodialysis. Int J Nephrol. 2021;2021. doi: 10.1155/2021/8876559. DOI: https://doi.org/10.1155/2021/8876559
AI-Rubaia ZR, AI-Ashour IA, AI-Mubarak ZA. Assessment of dialysis adequacy among hemodialysis patients. Int J Health Sci (Qassim). 2022;12507–12515. doi: 10.53730/ijhs.v6ns2.8213. DOI: https://doi.org/10.53730/ijhs.v6nS2.8213
Doan KVD, Nguyen HTM, Nguyen NTH, Dang KC, Yang SH, Van Duong T. Associations of socio-demographic, clinical and biochemical parameters with healthcare cost, health-and renal-related quality of life in hemodialysis patients: A clinical observational study. Int J Environ Res Public Health. 2020;17(18):1–15. doi: 10.3390/ijerph17186552. DOI: https://doi.org/10.3390/ijerph17186552
Barzegar H, Moosazadeh M, Jafari H, Esmaeili R. Evaluation of dialysis adequacy in hemodialysis patients: A systematic review. Urol J. 2016;13(4):2744–2749. doi: 10.22037/uj.v13i4.3314.
Fontao SM, Manso P, Audije-Gil J, Gascueña DH, Dapena F, Aresté N, et al. Quality of life and clinical data in hemodialysis patients with different degrees of pruritus. Sci Rep. 2025;15(1):6222. doi: 10.1038/s41598-024-83833-2. DOI: https://doi.org/10.1038/s41598-024-83833-2
Alqalah TAH, Alrubaiee GG, Alkubati SA. Factors associated with the quality of life and needs of hemodialysis patients in Saudi Arabia: A basis for improved care. Medicina (Lithuania). 2025;61(2). doi: 10.3390/medicina61020180. DOI: https://doi.org/10.3390/medicina61020180
Bujang Z, Rahman Ramdzan A, Tze Ping Pang N, Azzeri A, Jaafar H, Isahwan Ahmad Mulyadi Lai H, et al. Health-related quality of life among hemodialysis patients and its associated factors: A scoping review. Mal J Med Health Sci. 2023;19(Supp 20):240-249.
Hasan LM, Shaheen DAH, El Kannishy GAH, Sayed-Ahmed NAH, Abd El Wahab AM. Is health-related quality of life associated with adequacy of hemodialysis in chronic kidney disease patients? BMC Nephrol. 2021;22(1). doi: 10.1186/s12882-021-02539-z. DOI: https://doi.org/10.1186/s12882-021-02539-z
El-Sheikh M, El-Ghazaly G. Assessment of hemodialysis adequacy in patients with chronic kidney disease in the hemodialysis unit at Tanta University Hospital in Egypt. Indian J Nephrol. 2016;26(6):398–404. doi: 10.4103/0971-4065.168141. DOI: https://doi.org/10.4103/0971-4065.168141
Ghabisha A, AlShoaibi IA, Ahmed F, Ghabisha SA, Abdo B. Predictors of mortality among hemodialysis patients at Al-Thora General Hospital, Ibb Governate, Yemen: A retrospective study. Cureus. 2024; doi: 10.7759/cureus.65457. DOI: https://doi.org/10.7759/cureus.65457
Daugirdas JT, Depner TA, Gotch FA, Greene T, Keshaviah P, Levin NW, et al. Comparison of methods to predict equilibrated Kt/V in the HEMO Pilot Study. Kidney Int. 1997;52(5):1395–1405. doi: 10.1038/ki.1997.467. DOI: https://doi.org/10.1038/ki.1997.467
RAND Corporation. RAND Health, Kidney Disease Quality of Life Instrument (KDQOL). RAND Corporation; 2018. Accessed February 20, 2025. https://www.rand.org/health/surveys_tools/kdqol.htm
Hays RD, Kallich JD, Mapes DL, Coons SJ, Carter WB. Development of the Kidney Disease Quality of Life (KDQOLTM) instrument. Qual Life Res. 1994;3(5):329–338. doi: 10.1007/BF00451725. DOI: https://doi.org/10.1007/BF00451725
Jones CB, Bargman JM. Should we look beyond Kt/V urea in assessing dialysis adequacy? Semin Dial. 2018;31(4):420–429. doi: 10.1111/sdi.12684. DOI: https://doi.org/10.1111/sdi.12684
Kefale B, Alebachew M, Tadesse Y, Engidawork E. Quality of life and its predictors among patients with chronic kidney disease: A hospital-based cross-sectional study. PLoS One. 2019;14(2):e0212184. doi: 10.1371/journal.pone.0212184. DOI: https://doi.org/10.1371/journal.pone.0212184
Elamin S, E Elbasher AH, Ali SE, Abu-Aisha H. Arabic translation, adaptation, and validation of the kidney disease quality of life short-form 36. Saudi J Kidney Dis Transpl. 2019;30(6):1322–1332. doi: 10.4103/1319-2442.275476. DOI: https://doi.org/10.4103/1319-2442.275476
Goh Z, Griva K. Anxiety and depression in patients with end-stage renal disease: impact and management challenges – a narrative review. Int J Nephrol Renovasc Dis. 2018;11:93-102. doi: 10.2147/IJNRD.S126615. DOI: https://doi.org/10.2147/IJNRD.S126615
Correia J, Waqas A, Assal JP, Davies M, Somers F, Golay A, et al. Effectiveness of therapeutic patient education interventions for chronic diseases: A systematic review and meta-analyses of randomized controlled trials. Front Med (Lausanne). 2023;9:996528. doi: 10.3389/fmed.2022.996528. DOI: https://doi.org/10.3389/fmed.2022.996528
Suleiman AAQ, Abed SM, Ahmed SS. Assessment the Levels of Depression among Patients with Hemodialysis at the Dialysis Centers in Mosul City. Pak J Med Health Sci. 2023. doi: 10.53350/pjmhs202317867. DOI: https://doi.org/10.53350/pjmhs202317867
Saeed HS, Sinjari HY. Assessment of hemodialysis efficacy in patients with end-stage renal failure in the erbil hemodialysis center. Med J Babylon. 2018;15:276-280. doi: 10.4103/MJBL.MJBL_62_18. DOI: https://doi.org/10.4103/MJBL.MJBL_62_18
Kim S, Nigatu Y, Araya T, Assefa Z, Dereje N. Health related quality of life (HRQOL) of patients with End Stage Kidney Disease (ESKD) on hemodialysis in Addis Ababa, Ethiopia: A cross-sectional study. BMC Nephrol. 2021;22(1). doi: 10.1186/s12882-021-02494-9. DOI: https://doi.org/10.1186/s12882-021-02494-9
Bayoumi M, Al Harbi A, Al Suwaida A, Al Ghonaim M, Al Wakeel J, Mishkiry A. Predictors of quality of life in hemodialysis patients. Saudi J Kidney Dis Transpl. 2013;24(2):254-259. doi: 10.4103/1319-2442.109566. DOI: https://doi.org/10.4103/1319-2442.109566
Ralli M, Tsironi M, Panoutsopoulos G, Kolovos P, Aroni A, Zyga S. Sleep and quality of life in relation to dialysis adequacy in chronic kidney disease patients undergoing hemodialysis. Int J Caring Sci. 2022;15(3):1753–1763.
Prevyzi E, Argyriou G, Kollia T, Nestor A, Kotanidou A, Marvaki C. Estimating the quality of life of hemodialysis patients and adequate clearance. Health Res J. 2016;2(4). doi: 10.12681/healthresj.19847. DOI: https://doi.org/10.12681/healthresj.19847
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Al-Rafidain Journal of Medical Sciences ( ISSN 2789-3219 )

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Published by Al-Rafidain University College. This is an open access journal issued under the CC BY-NC-SA 4.0 license (https://creativecommons.org/licenses/by-nc-sa/4.0/).











